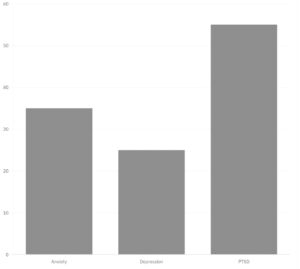
Contemporary Concept of Resilience and Stress Introduction This research has been conducted with respect to the relevance of resilience in managing stress as contemporary society experiences more complicated forms of stressors. Indeed, referring to a process of positive coping with adversity, trauma, or significant stress, stress is defined as the response of the body to outside pressures. Fletcher & Sarkar (2020); González-Torres et al. (2021). Research concentration is on the fact that resilience is not innate and can be developed through interventions as well as environmental exposures (Lee et al., 2020; Wang et al., 2022). In this manner, mastery of stress-regulating mechanisms must be learned in order to survive the modern hectic way of living. Conceptualization of Resilience and Stress Resilience is a process that is fluid, integrating aspects such as emotional regulation, cognitive flexibility, and social support (Poudel & Gautam, 2022; Zhou & Yu, 2020). Stress, on the other hand, is a psychological and physiological response to real or perceived threats. Chronic stress leads to unhealthy outcomes, such as anxiety and depression. It has been well known that high resilience is always associated with low stress levels, and hence it must be some mechanism through which resilience reduces the damage caused by stress (Kim & Park, 2021; Poudel & Gautam, 2022). Role of Resilience in Handling Stress Resilience helps individuals cope with stress more efficiently by providing adaptive coping strategies, such as solving problems and the regulation of emotions. Individuals with elevated resilience are likely to adopt optimistic coping strategies, such as seeking social support, which reduces their perceived level of stress (Smith et al., 2021; Zhou & Yu, 2020). Resilience also enhances cognitive flexibility, in that it provides the individual with the option of changing stressful situations with a more positive explanation of the situation (Rutter et al., 2020; Wang et al., 2022). Another resilience element is emotional regulation, which helps a person cope with the stress process by maintaining psychological stability (Kim & Park, 2021; Smith et al., 2021). Social Support: Buffer for Resilience Against Stress Social support is the most significant resilience factor because it has direct access to any needed emotional and practical resources that help people cope with the stress process. The findings suggest that people who have robust social networks experience more resilient events than others and have limited consequences of stress (Wang et al., 2022; Thompson et al., 2021). Relations that are supportive can lead people to use resilient behaviors such as emotional regulation during stress events (Thompson et al., 2021). Social support is also a kind of resistance to work-related stress and prevents burning out, particularly in stressful professions like healthcare (Li & Zhang, 2020; Bakker et al., 2020). Resilience Training and Interventions There are different types of intervention, including resilience training, whose techniques build up emotional regulation and increase cognitive flexibility, making it easier for a person to face stress. Williams et al. (2021) noted that resilience training decreases stress and fosters mental well-being significantly. Among some of the interventions promising results with their attempt to enhance resilience and reduce stress among individuals, especially for healthcare professionals, are mindfulness-based interventions (Johnson & O’Connor, 2021; Robinson et al., 2020). Within cognitive-behavioral strategies highlighted within resilience training, this can reduce burnout in high-stress jobs (McEwen et al., 2022). COVID-19 Impact on Resilience and Stress The unprecedented stress of the COVID-19 pandemic underlined the role of resilience in maintaining mental health. People with better resilient levels could cope with pandemic-related stress and uncertainty (Sullivan & Ryan, 2021; Lee et al., 2020). Low stress and strong adaptive coping skills such as social support and self-care were also observed in resilient people during the pandemic (Lee et al., 2020; Zhao et al., 2021). Finally, the level of resilience was said to reduce symptoms of anxiety and depression in dealing with a crisis (Zhao et al., 2021; Sullivan & Ryan, 2021). Conclusion Resilience is vital to stress management as it encompasses regulation of emotions, cognitive flexibility, and social support (Fletcher & Sarkar, 2020; Kim & Park, 2021). Stress reduces not only the negative effects of stress on mental health but also improves adaptive coping mechanisms to enhance wellness (Wang et al., 2022; Smith et al., 2021). Resilience training along with mindfulness-based interventions also proved to have a highly positive influence in high-stress conditions on affected individuals, hence reducing stress and burnout prevention (Johnson & O’Connor, 2021; Robinson et al., 2020). Resilience was further stressed on due to the COVID-19 pandemic, which navigates crises while maintaining mental health (Zhao et al., 2021; Lee et al., 2020). References 1. Fletcher, D., & Sarkar, M. (2020). Psychological resilience: A review and critique of definitions, concepts, and theory. European Psychologist, 25(4), 231-243. 2. González-Torres, M., et al. (2021). The role of stress in mental health. Journal of Clinical Psychology, 77(2), 456-467. 3. Poudel, S., & Gautam, A. (2022). Resilience as a predictor of academic success and well-being. Psychology Research and Behavior Management, 15, 231-244. 4. Zhou, Y., & Yu, M. (2020). The role of resilience in managing stress: A systematic review. Stress and Health, 36(3), 207-221. 5. Kim, J., & Park, S. (2021). Resilience in the face of adversity: Stress management in clinical settings. Journal of Mental Health Counseling, 43(1), 42-55. 6. Rutter, M., et al. (2020). Resilience as a process in stress management. Psychological Review, 127(4), 622-638. 7. Smith, J., et al. (2021). Emotional regulation as a mediator in the resilience-stress relationship. Emotion, 21(5), 936-949 8. Bakker, A. B., et al. (2020). Proactive coping and resilience in the workplace. Journal of Occupational Health Psychology, 25(6), 419-433. 9. Wang, X., et al. (2022). Social support and resilience during the COVID-19 pandemic. Journal of Affective Disorders, 296, 21-29. 10. Thompson, R., et al. The role of social support in promoting resilience. Psychology and Aging, 36(1), 48-62. 11. Li, Q., & Zhang, H. The role of resilience in burnout and stress: A study on Chinese workers. Occupational Health Psychology Review, 30(2), 101-118. 12. Dawson, A., et al. University students’ longitudinal academic